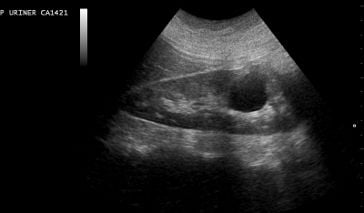
Cystic kidney disease is a general classification for a group of similar (heterogeneous) disorders that result in the development of cysts on the kidney. Kidney cysts are abnormal sacs that can be filled with fluids, gases or solids. These pouches can be microscopic, requiring no treatment. Or, they can be quite large, significantly impacting the function of one (unilateral) or both (bilateral) kidneys. While the kidneys are predominately affected in cystic kidney disease disorders, the liver, pancreas, brain, and areterial blood vessels may also be impacted.
Cystic Kidney Disease Causes
Kidney cysts can be hereditary, meaning they are passed down in families. The inherited disorders occur when genetic abnormalities cause defects with the structure and function of the kidney(s). But renal cysts may also be acquired (nonhereditary), developing as the individual ages or making a formal appearance either in childhood or later in life. In both hereditary and nonhereditary cases, the cysts replace normal, healthy kidney tissue. As this happens, kidney function decreases, and can ultimately lead to kidney failure.
Types of Cystic Kidney Disease
Hereditary cystic kidney diseases include:
- Autosomal dominant polycystic kidney disease (ADPKD): ADPKD is the most common cystic kidney disease, occurring in one out of every 400-1,000 people. It typically presents in adulthood and causes a number of fluid-filled cysts to grow on the kidneys. Roughly half of those with this condition will develop end-stage renal (kidney) disease and need a kidney transplant or dialysis. This systemic disorder mainly affects the kidneys, but may impact the liver, pancreas, brain and arterial blood vessels as well. Symptoms, which can range from mild to severe, include abdominal pain, high blood pressure, blood in the urine and urinary tract infections. These signs usually do not appear until adulthood, between the ages of 30 and 60.
- Autosomal recessive polycystic kidney disease (ARPKD): This condition occurs most often in infancy and childhood. Here, multiple fluid-filled cysts form in the inner and outermost part of the kidneys, causing its tubules and ducts to become severely dilated. As a result, ARPKD often leads to kidney failure by the time the child has reached the age of 10, requiring dialysis or transplantation to improve their chance of survival. This form of polycystic kidney disease has a poorer prognosis, with between 23-30 percent of those with ARPKD dying within the first few hours or days of birth, mainly because of breathing difficulties caused by having underdeveloped lungs, which can be attributed to a deficiency of amniotic fluid while in the womb. Those who live longer often have enlarged kidneys within the first month, which impairs the organs' ability to remove waste from the body. In roughly 50 percent of cases, the liver is enlarged and damaged too.
- Medullary cystic kidney disease: Medullary cystic kidney disease is a rare genetic disorder that leads to end-stage renal disease. There are two forms of the disease: type 1 and type 2. Type 1 has a later age of onset (median age 62), while type 2 develops earlier in life (median age 32). This autosomal dominant kidney disorder is characterized by cysts in the center of both kidneys, as well as tubulointerstitial sclerosis. As a result, the kidneys become scarred and begin to steadily lose their ability to function.
- Von Hippel-Lindau (VHL) disease: This condition is an unusual genetic disease that affects one out of every 36,000 newborns in the United States. It is distinguished by the formation of tumors (hemangioblastomas) and cysts (fluid-filled sacs) that can grow in the kidneys, pancreas, brain, spinal cord and genital tract (in men). The tumors, which often appear during young adulthood, can be either benign or cancerous. Still, those with VHL are at greater risk of developing kidney cancer.
- Tuberous sclerosis complex (TSC): Tuberous sclerosis complex, also known as Bourneville disease, is a multisystem disorder that causes nonmalignant tumors to grow in the brain and other vital organs, like the kindeys. The condition occurs because one of two genes (TSC1 and TSC2) have been altered and no longer properly code for the proteins (tuberin and hamartin) that operate as tumor growth suppressors. Symptoms vary based on the location of the tumors, but include seizures, behavioral problems, skin abnormalities, mental retardation and lung and kidney disease. In patients with TSC, kidney cysts are common.
Nonhereditary cystic kidney diseases can result because of an injury or disease that impacts the kidney. Examples include:
- Acquired cystic kidney disease (ACKD): This condition occurs when multiple fluid-filled cysts develop on one or both kidneys and there is no evidence that the cysts are hereditary. Men are three times more likely to develop this condition than women. However, doctors do not know why the gender is more susceptible to the disease. ACKD typically develops in patients that experience kidney failure. Approximately 20 percent of patients with kidney failure develop this condition before beginning dialysis. Another 60 percent of patients with kidney failure develop ACKD within four years of starting dialysis. Generally, the cysts that develop are harmless and do not require any treatment. If symptoms do develop they typically include: infection of the cysts, which causes back pain; or bleeding of the cysts, which causes blood in the urine.
- Medullary sponge kidney: Medullary sponge kidney, also known as Cacchi-Ricci disease, is a benign condition that typically increases a patient’s risk of kidney stones and urinary tract infections. The prevalence of the condition in the general population is one in 5,000 persons. The condition develops because of a defect in the tubules of the kidney that carry urine. Cysts that form in the tubules reduce the flow of urine, allowing waste products such as calcium to build up in the kidneys. Increased waste products can lead to the formation of kidney stones or infections.
- Multicystic dysplastic kidney (MCDK): This condition occurs because of a malformation of the kidney during fetal growth. The affected kidney has no functional renal tissue and instead is comprised of cysts/scar tissue. It can not carry out its task. Typically, MCDK only affects the function of one kidney. Patients with one healthy kidney and one kidney with MCDK are monitored to ensure that the healthy kidney functions normally and the diseased kidney does not cause any adverse health issues. If the patient develops renal hypertension or malignancy, it is surgically removed.
- Localized renal cystic disease: This condition typically causes the development of numerous benign cysts on one kidney (unilateral), with no cysts on the other kidney or other organs. The tumors may impact the entire kidney or just a portion. Patients with this condition often have no symptoms. If symptoms develop, the patient may experience blood in the urine and flank pain. It is unclear why localized renal cystic disease develops.
Cystic Kidney Disease Symptoms
Cystic kidney diseases often do not cause any symptoms for the patient. If there are no symptoms, cystic kidney diseases may be detected during the diagnosis of another medical condition. However, if symptoms develop they can include:
- Renal colic (excruciating pain in the region on the back between the ribs and the hip)
- Recurrent urinary tract infections
- Blood in the urine (hematuria)
- Back or flank pain
- Headache
- Fever/chills
- Upper abdominal pain and swelling
- Kidney stones
- High blood pressure (hypertension)
- Kidney failure
- Frequent urination
Diagnosing Cystic Kidney Disease
Cystic renal diseases must be diagnosed by a doctor. If there are symptoms of the condition, the doctor will complete a physical exam and gather the patient's health history to determine if the condition may be hereditary. In addition, the doctor may use various imaging procedures to visualize the cysts including:
- Ultrasound: An ultrasound uses sound waves that are bounced off of organs in the body to create a picture on a monitor.
- Computerized tomography or CT scan: CT scans use X-rays to create a three dimensional picture of organs inside the body. The doctor may inject a contrast dye into the patient’s vein to better visualize the kidneys.
- Magnetic resonance imaging (MRI): MRIs use radio waves and magnets to provide three dimensional images of organs inside the body.
Cystic Kidney Disease Treatment
Cystic kidney disease treatment depends on whether symptoms exist and if so, how severe they are. If cystic renal disease is not causing any symptoms and is not impacting the function of the kidney, no treatment may be required. Conditions that result from the cysts, such as urinary tract infections and kidney stones, will require antibiotics or surgery. Cysts that cause pain can be drained by inserting a needle and drawing out its contents. Patients with cysts are typically monitored to detect their development and look for signs of cancer. Surgery may be needed to stop the sacs from bleeding. Cysts can result in renal failure, requiring dialysis or renal transplant.
References
Acquired cystic kidney disease. (2012). National Kidney and Urologic Diseases Information Clearinghouse. NIH Publication No. 09-6403
Katabathina, V.S., Kota, G., Dasyam, A.K., Shanbhogue, A.K.P., & Prasad, S.R. (2010). Adult renal cystic disease: A genetic, biological and developmental primer. RadioGraphics, 30, 1509-1523.