The prostate, which is located below the bladder and wraps around a section of the urethra, is a walnut-sized reproductive gland responsible for producing a milky fluid that makes up the majority of the male ejaculate. Prostate cancer occurs when cells in the prostate mutate and grow out of control--most often, it's the cells in the gland (not the muscle) of the prostate, a type of cancer referred to as adenocarcinoma.
The disease spreads at different rates in different people: While it develops quite rapidly in some men, others can have the disease for many years yet die of other causes. And some men can die of the disease after experiencing no symptoms whatsoever.
Risk Factors for Prostate Cancer
Prostate cancer is one of the most prevalent cancers in men. Risk of disease increases with age, and it is most prevalent in men over 65.
Obesity and family history also increase risk. So does ethnicity: The disease is more than twice as prevalent in African American than Caucasian men.
Causes of Prostate Cancer
While researchers know that abnormal cell development is a result of DNA mutations, and that these mutations are at the root of cancer development, the instigating factors have not been fully uncovered. Mutated cells divide rapidly, allowing them to accumulate into tumors and take over nearby tissue. When cells break off, they spread through blood and lymph vessels and can metastasize in different regions of the body.
Prostate Cancer Symptoms
Because the prostate is located below the bladder, one of the main indicators of prostate health is urine flow. Weak, interrupted, or frequent urination (particularly at night) can all indicate a prostate issue. Difficulty urinating, painful urination, or a burning sensation may also be symptomatic.
Additional symptoms can include consistent pain in back, hips or pelvis, as well as blood in urine or semen, or pain during ejaculation. Most of these can also indicate other urinary-tract problems, however, so contact a physician when experiencing any of these symptoms.
Prostate Cancer Diagnosis
Screening:
There are two primary prostate screening tests:
- Digital rectal exams are physical exams, in which a doctor wears lubricated gloves and uses a finger (or "digit") to search for any distinctive signs in the size, shape or texture of the prostate.
- Prostate specific antigen (PSA) is a protein produced by the prostate, measurable with a blood test, and high levels may indicate the presence of prostate cancer. However, since high levels can also indicate other conditions, such as prostatitis, the American Urological Association suggests that the test should be reserved for men over 40: Men who are at high risk (African Americans and those with a family history of the disease) should start getting the test at age 40, and men between the ages of 55 to 69 should only be screened every two years. (High PSA levels have led to an unreasonable number of false positives and unnecessary prostate biopsies.) The PSA test is also used to measure prostate cancer-treatment effectiveness, and is the most sensitive tool for doing so.
If these screenings detect abnormalities, further testing may be required to rule out prostate cancer. These tests include:
- Transrectal ultrasound, uses a small probe placed in the rectum that creates an image of the prostate. This is an outpatient procedure done in a doctor's office that normally takes less than 10 minutes.
- Prostate biopsy, in which a small sample of prostate tissue is gathered and then analyzed for the presence of cancerous cells. An ultrasound is used to guide small needles through the rectum to the prostate. The procedure takes about 30 minutes.
Grading and Staging Prostate Cancer
If a biopsy confirms the presence of cancerous cells, the next step is to grade the cancer by determining its aggressiveness. During this process, the tissue samples are analyzed alongside healthy prostate cells. The more aggressive the cancer, the higher the grade. On a scale of two to ten, a Gleason Score of 2 means the cancer is not aggressive and the cancerous area looks similar to normal tissue. A Gleason Score of 10 has the worst prognosis.
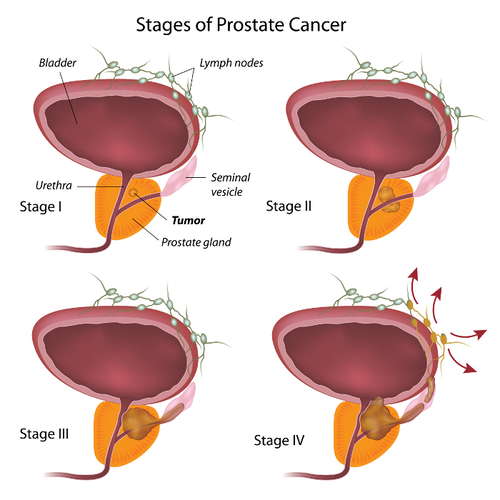 If the physician has reason to believe that the disease has spread, she will order a bone scan, an ultrasound, a CT scan, and/or an MRI in order to stage the cancer. The stages are defined as:
If the physician has reason to believe that the disease has spread, she will order a bone scan, an ultrasound, a CT scan, and/or an MRI in order to stage the cancer. The stages are defined as:
- Stage I prostate cancer is considered early cancer, and is generally limited to only a small portion of the prostate. Stage I cancer cells are not considered aggressive.
- Stage II prostate cancer can either indicate aggressive cells and small relative size, or larger size. At this stage, it is possible that the cancerous cells have enveloped both sides of the gland.
- Stage III prostate cancer indicates that cancer has spread. At this stage it may have metastasized from the prostate gland to other tissues or to the seminal vesicles.
- Stage IV prostate cancer refers to cancer that has developed beyond the gland. At this point it is likely to have spread or metastasized to other organs. Affected organs can be the bladder, lymph nodes, lungs, bones or other possible organs.
An oncologist will use information about the cancer's grade and stage to determine the best treatment plan.
Prostate Cancer Treatments
Treatment for prostate cancer depends on the aggressiveness of the disease, the extent of its spread, and the patient's overall health.
In some cases, a physician will recommend watching and waiting, an approach also known as 'active surveillance.' This requires regular blood tests, rectal exams, and/or biopsies to ensure the cancer is not advancing. For cancer that has progressed, treatment can include radiation therapy, hormone therapy, surgery, chemotherapy, freezing, or heating. (For more information on these approaches and their side effects, see Prostate Cancer Treatments and consult a doctor.)
References
1. Li J, German R, Tai E, et al. Recent trends in prostate cancer testing and incidence among men under age of 50. Cancer Epidemiology [serial online]. April 2012;36(2):122-127.
2. Grimm P, Billiet I, Zietman A, et al. Comparative analysis of prostate-specific antigen free survival outcomes for patients with low, intermediate and high risk prostate cancer treatment by radical therapy. Results from the Prostate Cancer Results Study Group. BJU International. February 2, 2012;109:22-29.